The word of the day is "arbitrage".
Officially, Merriam-Webster defines the English language word "arbitrage" this way: "The nearly simultaneous purchase and sale of securities or foreign exchange in different markets in order to profit from price discrepancies". However, arbitrage does not exclusively apply to securities sold on Wall Street. The term has also been appropriated by the Pharmacy Benefit Manager ("PBM") industry.
But PBM's are not Wall Street investment banks. And that's something we all need to realize.
 |
| Image courtesy of Harvard Business School |
The PBM Accountability Project 2021 report "Understanding the Evolving Business Models and Revenue of Pharmacy Benefit Managers" (download their highly informative report by visiting HERE) defined the term "arbitrage" this way:
"PBMs' lack of transparency is critical to their operations and allows them to buy a product (or service) [such as a drug or biologic medicine] from one stakeholder in the system and re-sell that product (or service) to another stakeholder at a significantly higher price, all without the payer understanding the true cost or inflationary nature of the services they have just purchased — a practice [euphemistically] referred to [by the PBM industry] as 'arbitrage'".
Adam Fein, President of Pembroke Consulting and another entity he calls The Drug Channels Institute described the situation this way when he observed how a surprising majority (74%) of GoodRx customers actually have a drug benefit provided by insurance. He wrote (see his post at https://www.drugchannels.net/2021/03/how-goodrxs-rapid-growth-creates.html for details):
"Incredibly, three out of four consumers who used GoodRx already had commercial, Medicare, or Medicaid insurance. This means that someone — the consumer, their employer, and/or the government — paid insurance premiums for a pharmacy benefit managed by a PBM. Yet it was still worthwhile for people to bypass their plan's out-of-pocket costs and PBM network rates in favor of a different PBM's rates ... such arbitrage creates potent conflicts between PBM's and their plan sponsor clients".
Adam Fein also included this image which comes directly from GoodRx:
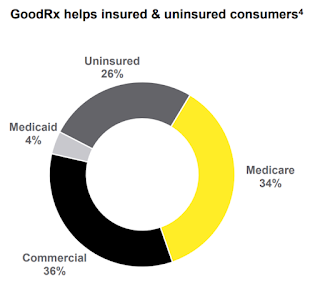 |
| GoodRx 2020 Payer Mix |
In a separate post about GoodRx and its disruptive impact on the pharmacy business (see HERE), Adam Fein further observed:
"Discount cards succeed by enabling people to arbitrage network pharmacy rates across PBM's."
He adds:
"...benefit designs and network rates can differ among PBM's. This difference can allow a patient to reduce their out-of-pocket expenses by accessing the rates of another PBM — or maybe even another network from their own plan's PBM — by using a discount card."
PBM Arbitrage Is A Clever Term to Describe Ripping-Off Both Pharma and Patients
According to a 2018 White Paper (see https://healthpolicy.usc.edu/wp-content/uploads/2018/03/2018.03_Overpaying-for-Prescription-Drugs_White-Paper_v.1.pdf for the paper) published in March 2018 by the University of Southern California's Schaeffer Center for Health Policy and Economics, about one-quarter of the time patients visit the pharmacy counter, prescription drugs end up costing them MORE money when paying with insurance than just paying with cash. Of course, depending on your employer's benefit design, that could potentially be true more frequently than one quarter of the time (I've been covered by some plans where it was true 100% of the time until the deductible was satisfied; hence it was true for about half the year in that situation). Bypassing your own insurance company's pharmacy benefit to save a LOT of money on prescriptions defies what we've been taught, and yet a growing body of data suggests it is happening more and more.
Of course, paying "cash" is further complicated by PBM arbitrage.
Paying cash often includes using various readily-available discount coupons (including PBM-powered coupons such as those from GoodRx, or any number of rivals such as SingleCare which I'll tell you about, as well as manufacturer coupons from the pharmaceutical companies) to reduce YOUR prices which may or may not always work with your insurance or Medicare, but the point is you could be paying too much by using your insurance (including Medicare), and that happens at least 25% of the time.
But It Counts Towards My Deductible ... Right?
The single biggest myth is that patients should simply tolerate paying artificially-inflated list prices for prescription drugs because they mistakenly believe doing so contributes meaningfully towards reducing the deductible they must satisfy.
That's a falsehood which you need to forget about.
In reality, insurers only credit covered patients for the deeply-discounted prices their PBM's negotiate on their behalf, not the bloated cash list prices patients are charged at the pharmacy for prescription drugs. One trouble is that covered patients really have no idea of how much credit each drug purchase is being applied towards their deductibles. Your health insurance company is keeping that information secret from you. That lack of disclosure is key.
That makes shopping for prescription drugs in the U.S. an unnecessarily complicated decision-making process. The real issue is that patients never really know what the price will be until we get to the pharmacy checkout counter (although you can ask a pharmacy tech before-hand, but its time-consuming).
You should consider using discount cards for prescriptions that are either not covered by your insurance at all because its not on the preferred drug formulary for your insurance plan, or for medications in which using your insurance prior to satisfying any deductible will be more expensive using your insurance card.
The PBM Accountability Project report again described the situation this way:
"Excess complexity in the U.S. prescription drug distribution system and information asymmetry in the market currently prevents patients and payers from properly evaluating PBM decisions which directly impact them."
There are, of course, various other factors to consider.
For example, if you have deductibles to satisfy before pharmacy benefits go into effect, then you may directly experience this corrupt form of "arbitrage" annually (usually on January 1, although some plans reset their deductibles on their plan anniversary date) when deductibles are reset to zero.
I find it helpful to try a simple sanity-check if the price you're being asked to pay just "seems" like it makes sense to bypass your insurance. I experienced this bizarre arbitrage on prescription drug pricing dynamic earlier this year.
My spouse uses a generic hypertension drug (the name of the drug was eplerenone 50 mg tablets). Using our insurance to buy the drug, insurance and its PBM Caremark had charged $48.40 for a 30-day supply of a generic drug which is very literally "Made in India".
That was not OK.
I understand that many drug companies now make drugs offshore because it earns them even more (according to researchers, 40-50% of the nation's generic prescription drug supply comes from India these days because it enriches the pharmaceutical industry), but that was still an unreasonable cost of $1.61 per tablet! In my gut, I just KNEW we were being ripped off. In other cases, it may not be so certain. In which case, I would suggest you use your best judgement. It may be worth several hours of your time to shop around.
One good resource to check is the Medicaid National Average Drug Acquisition Cost (NADAC) website at https://data.medicaid.gov/nadac. NADAC is the Centers for Medicare and Medicaid Services' (CMS) estimate of the national average drug invoice price paid by independent and retail chain pharmacies, NADAC excludes specialty and mail order pharmacies, and does not reflect any rebates, price concessions, or off-invoice discounts. CMS randomly surveys retail pharmacies to determine NADAC. Out of approximately 67,000 U.S. pharmacies, CMS selects 2,500 pharmacies per month and approximately 450-600 pharmacies voluntarily respond with actual drug price data. The website enables you to download a spreadsheet with nearly every NDC sold in the U.S. I search for the generic drug name to save myself some time. For generic drugs, there may be 10 or 12 different NDC numbers for each potency (such as the number of milligrams of the drug) and provides a per unit cost (such as a 10 mg tablet and the cost is on a per-pill basis). Usually, the NDC prices for all of the same potency of each drug are priced identically, but not always. If you really want to be specific, look at the drug label your pharmacy gives you and find the actual NDC number. Or you can simply average all of them and that will provide a good ballpark number and cost. If the price your insurance company's PBM gives you is much higher (as mine was), you're being ripped off and your next step is to find a place where you can buy the drug for less, using coupons if necessary to reduce your price.
Sanity Check: Generic Drugs Made Offshore Should NOT Cost Us More Than $1/Tablet
Since we still had several refills before the next doctor's appointment, in our case, I first searched for coupons to at least reduce our out-of-pocket price. Oddly, many generic drugs now have coupons; we were taught generics are a way to save money, but now they are a way for PBM's to mark up prices without anyone knowing.
Weird Glucagon Example
Consider this: one of several generic glucagon emergency kits which are now FDA-approved can be purchased, including one for a mere $5 with a co-pay coupon from the generic drug manufacturer Fresnius Kabi USA whose U.S. base is located in suburban Chicago. The parent company is based around Frankfurt, Germany.
But the odd PBM "arbitrage" has influenced patient prices in a very negative way.
The bogus list price for a Fresnius Kabi USA Glucagon Emergency Kit https://glucagonemergencykit.com/ without the manufacturer co-pay coupon is a stunningly uncomfortable $260.47 at CVS or $245.03 at Walgreens according to GoodRx.
This is the second generic glucagon emergency kit approved by the FDA in 2020 (the first was from California-based Amphastar Pharmaceuticals), yet the price on those generics is MORE expensive than old-school glucagon kits from Lilly or Novo Nordisk sell for which defies logic. Get a coupon for the Fresnius Kabi USA Glucagon Emergency Kit at https://glucagonemergencykit.com/index.php/information-for-caregivers/assistance-program/ — just pay very close attention to the mice-type on the coupon disclosure, because the coupon only works for commercial healthcare insurance claims, or alternatively cash-payers subject to monthly cap of $125 and separate annual maximum cap of $1,500. The impact is that it will only mark the price paid down by $125 for any one purchase, which makes it critical to buy it at the pharmacy that sells it for the lowest price.
I was able to use a SingleCare coupon (which are discounts provided by the pharmacy itself, rather than via a PBM) and buy one at Rite Aid pharmacy for a price of just $56.66. Then, I used the manufacturer coupon from Fresnius Kabi USA which brought my price down to just $5. That was a price I'd expect to pay for a generic. Oh, and did I mention that I completely bypassed my insurance?! Considering my insurance company PBM expected me to pay like $260 for that product, that was insane.
Just Not for Medicare? But Only if You Tell Pharma or PBM's.
Medicare patients are technically exempt from using many of the manufacturer and PBM discount coupons, and patients will be asked to reveal to the drug company (or the PBM) that they are "NOT enrolled in a governmental program".
But no law requires patients to tell the drug company or PBM how they will actually be paying for a drug; it's none of their business and they are not entitled to know that. Coupons and Medicare don't mix. But patients can simply answer that they're not enrolled in government healthcare program to pay for the drug, because no federal law (and I'm not aware of any state laws) that entitles a PBM to ask for that information, or obliges patients to answer the question truthfully.
None.
The drug companies and PBM's ask you for the information anyway and try and suggest they are entitled to that info, but they really are not. No law requires patients to answer the "eligibility" questions truthfully. They cannot prosecute patients for fraud because they are paying cash instead of submitting it as a Medicare Part D claim. Patients should be suspicious about telling a third-party how they'll be paying; after all, as long as they are being paid (and they ARE being paid), why should they care? Patients simply cannot use their Medicare card to pay for the drug at their pharmacy and also use the discount coupons, and that's fine.
With a SingleCare coupon, the price for a Fresnius Kabi USA generic glucagon kit was just $56.66 from a Rite Aid pharmacy. SingleCare coupons discounts are from the RETAILER, not a PBM or manufacturer, which means you may also be able to use a manufacturer coupon on the same purchase. If you don't have a Rite Aid pharmacy near you, its also possible (and maybe preferable given the price difference) to use the virtual online pharmacy known as Capsule pharmacy and buy it for a price for $48.42 which is even cheaper, and then use a Fresnius Kabi USA KabiCare coupon to buy it for just $5 out-of-pocket. With prices like that, there's no reason to use insurance or Medicare to pay for it. Using that method, patients would also likely not encounter the manufacturer coupon cash limit at all. They'd pay just $5 for it.
That's quite literally turning PBM "arbitrage" on its head.
And, no, it's not illegal.
I've heard stories that patients sometimes find it easier to pay cash and use coupons at one pharmacy (say Walgreens or Rite Aid), and then fill regular scripts with Medicare at a completely different pharmacy like CVS. That makes it easier on the pharmacy staff who won't mistakenly try to submit a purchase as a Medicare claim. Its just sad when generic drugs push patients into the Medicare drug "donut hole", yet our elected lawmakers in Congress have enabled this bizarre type of unethical PBM arbitrage to happen. Perhaps the U.S. FTC will finally crack down when its formal investigation into PBM wrongdoing is completed. I certainly hope so.
Back to Our Rx Markdowns
Anyway, for my spouse's generic hypertension drug, I did find a discount coupon to reduce the price on a site called InsideRx (which also has an app). I later learned InsideRx is owned/operated by the giant PBM owned by Cigna known as Express Scripts (under its "Evernorth" business unit). That also explains why the prices are lowest using Express Scripts Cash-Pay Mail Order Pharmacy by InsideRx compared to other pharmacies in its own network. Using that coupon with our insurance slashed $10 off the price Caremark intended to charge us, which reduced our price down to $38.40 for a 30-day supply. The realized cost was still a stunningly high $1.28/tablet, which was very expensive for a generic drug imported from India, although it brought a bit of temporary relief of 14% off the marked-up price Caremark said we should pay. And, I used their biggest rival to do it. However, I realized that still wasn't great for a generic drug made in India. The cost of generic drugs should usually be considerably less than $1 per tablet (like $0.50 to $0.70 per tablet).
Low and behold, I then discovered Caremark's PBM rival Cigna's Express Scripts offered an even lower price using its cash-pay mail order pharmacy and an InsideRx coupon. But I had to bypass our insurance to do it. So I did just that. I later learned that Aetna would only credit us for $7.50 for the drug, so the decision to simply bypass our insurance made financial sense. Express Scripts Cash-Pay Mail Order Pharmacy by InsideRx does have some peculiarities. For example, it only accepts e-scripts, so on the next appointment with the doctor, we asked them to send an e-script for the same drug to Express Scripts. That move not only got us a 90-day supply of the drug for a lot less money (it saved us a stunning 82% off the $48.40 our own PBM Caremark intended to charge us for the same medicine). Our price ended up being $25.39 for 90 tablets (that's 3x as much medicine), and that price didn't even require insurance. It's just sad that our own insurance was screwing us financially that way and they get away with it all the time.
HOW I Searched to Save 82% on Rx Drugs
Searching for lower prescription drug prices requires an investment of your time. The most significant cost savings on Rx drugs is often for those used on a chronic basis (not that it doesn't work for drugs taken to treat acute illnesses, its just that the savings will be for short-term meds prescribed for acute conditions may not be worth the extra effort unless the price is very high because you will fill it once, and then be done with the treatment). Nine of the sites are PBM-powered coupons which is essentially saving money with the parties responsible for runaway prices in the first place. One of the sites is one whereby the site works out discounts with the pharmacies directly.
To find the best prices, you really need to search ALL of the following websites/apps.
Also, be prepared to patronize different pharmacies for different drugs. Try to view them as transaction-oriented purchases which you can switch when it personally benefits you. The cost-savings can make a small amount of effort well worth the effort (sometimes using different mail-order pharmacies which is easier than going to multiple pharmacies all around town). I invested a Sunday afternoon price-shopping for prescription drugs. Finally, beware: these rules usually only apply for prescriptions which have lost their patent protection. For newer drugs still protected by patents, the best option for discounts may be coupons from the drug manufacturers. Just beware of the unique eligibility requirements for certain manufacturer discount coupons. For example, some manufacturer coupons may require a claim to be submitted to a commercial healthcare insurance plan in order to work (in which case, the coupons may not work with Medicare claims, and sometimes [but not always] coupons may not work for cash-payers).
Key is to read the fine-print on the coupon carefully (get your magnifying glasses out).
WHERE I Found Savings of 82% on Rx Drugs
Here is my comprehensive list; search ALL of the sites carefully and let price drive your purchase decisions.
GoodRx https://www.goodrx.com/ The proverbial elephant in the room of prescription drug price comparison and coupon-generating websites/apps is GoodRx Holdings, Inc. which describes itself as a "health technology company" based in Santa Monica, California. The company was described as a "unicorn" when it went public in September 2020. At the time of its IPO, GoodRx's adjusted net income — earnings before interest, taxes, depreciation, and amortization (EBITDA) was an impressive 40%. It also had $388M in 2019 revenue and $139M in operating profit at the time of its IPO. GoodRx has non-exclusive contracts with several different PBM's, including MedImpact, Cigna's Express Scripts, United Healthcare's OptumRx, and Navitus (which is a PBM owned by the nonprofit hospital chain SSM Health & warehouse wholesaler Costco). In April 2021, GoodRx also acquired a rival coupon website/app known as RxSaver https://www.rxsaver.com/ by RetailMeNot from Vericast which previously ran RetailMeNot. However, the reason any one coupon-generating website/app including GoodRx cannot always offer the lowest prices is because each only offers access to a single prescription drug formulary offered by each PBM, and most PBM's offer multiple drug formularies. For example, the PBM known as Express Scripts' biggest formulary (which reportedly covers more than 28 million lives) is a high-price/high-rebate formulary known as the National Preferred Formulary (NPF). But rival InsideRx accesses a different drug formulary called the Express Scripts National Preferred Flex Formulary with lower prices on many generic drugs. To find lower prices, you are basically FORCED to shop other websites/apps.
SingleCare https://www.singlecare.com/ Of all of the Rx price comparison/coupon-generating websites/apps, Boston-based SingleCare is currently unique among coupon-generating websites/apps in that it contracts directly with major pharmacy chains to negotiate discounted cash prices rather than using a PBM or combo of PBM's. Avoidance of paying a PBM a transaction fee on each prescription sale enables them to share some of the savings with patients directly. SingleCare has pricing deals with Walgreens, Walmart, CVS, Kroger as well as Rite-Aid. In total, the company reportedly has about 8,200 retail pharmacies/stores throughout the U.S., which represents over half of all the pharmacy locations in the country.
MedImpact Healthcare Systems, Inc's. is a San Diego-based PBM which is currently the giant HMO Kaiser Permanente's PBM. Its status as "last man standing" status as one of the last/only remaining independent PBM's not owned outright by a healthcare insurance company (although it is [or WAS] de facto controlled by its largest client: Kaiser Permanente; but note that in early 2022 Kaiser announced plans to drop MedImpact in favor of Express Scripts effective in 2023), it was also among the earliest PBM's to spot Rx drug sales opportunities with prescription drug coupon websites/apps. As a result, MedImpact works with virtually all of them. ScriptSave WellRx https://www.wellrx.com/, AmericasPharmacy https://www.americaspharmacy.com/ and BlinkHealth https://www.blinkhealth.com/ is each "powered" by the PBM MedImpact (the first two of these three are actually owned/operated by MedImpact) to deliver prescription drug pricing info. and discount coupons. Rival GoodRx also counts MedImpact as one of its non-exclusive PBM's, and MedImpact also helps to power McKesson's ScriptHero website/app. I don't think you need to check all three of them (WellRx, AmericasPharmacy and BlinkHealth), but I do recommend including at least one in your online shopping.
InsideRx https://insiderx.com/ Previously, I noted Cigna's Express Scripts which operates the InsideRx coupon-generating site/app whose prices cannot be found on GoodRx but notably also includes low prices for Express Scripts Cash-Pay Mail Order Pharmacy by InsideRx https://www.express-scripts.com/insiderx/#/ which is accessible by anyone whether they have insurance or not, or if their pharmacy benefits are managed by a different PBM (as mine was, being managed by Caremark). Due to self-preferencing, Express Scripts may be the low-price leader on certain generic drugs. Should that change, I have no problem buying elsewhere. While generic drug prices are frequently very low, there are some quirks to using the site/app: for example, it only accepts e-scripts from doctors. As noted, Express Scripts Mail Order Pharmacy drug pricing is not offered via rival sites/apps such as GoodRx, therefore if one wants access to generic drug prices from Express Scripts via coupons (which are occasionally the lowest prices available anywhere), they will need to search InsideRx. Express Scripts' InsideRx tool is slightly cumbersome to use (for example, searches must be done separately for both generic and branded drug names, and the site/app does not enable patients to sort the search results from lowest prices to highest). Still, due to self-preferencing, its own mail order pharmacy often comes in as the lowest-price offering on a number of generic drugs when purchased directly from the Express Scripts Cash-Pay Mail Order Pharmacy by InsideRx https://www.express-scripts.com/insiderx/#/ compared to other pharmacies within its own retail network.
OptumPerks https://perks.optum.com/ Rival United Healthcare's OptumRx PBM unit (or simply "Optum") operates the OptumPerks price comparison/coupon-generating website/app. It's basically a rebranded version of the old SearchRx which no longer operates its own brand. Some patients say that in terms of prices, OptumPerks frequently omits a large number of very heavily-rebated brand-name prescription drugs completely, hence rivals may offer better prices on those drugs. That said, Optum occasionally offers lowest prices on certain generic drugs which OptumRx sells very large volumes, although the company recently raised its prices on statin drugs by 45% (I previously paid just $15 for 90 tablets), hence Mark Cuban's CostPlus Drug Company or Costco pharmacy are now the clear low-price leaders on those at a cost of about $21 for 90 tablets. Still, OptumPerks is worth checking. As with rival Cigna Express Scripts InsideRx, sometimes, to get the lowest prices, patients may need to purchase the drugs using Optum's mail order pharmacy known as Optum Store https://store.optum.com/ to attain the lowest pricing on those particular generic drugs. Unlike rival Express Scripts which only accepts e-scripts, patients can actually mail their paper scripts into Optum Store which is an added benefit. In essence, one never knows if and when OptumPerks/OptumRx might enable better-priced offerings, so it should be included among those you search.
WellCardRx https://wellcardrx.com/ A smaller PBM known as Welldyne Rx, Inc. (and its subsidiary WellDyneRx LLC), much like its bigger PBM rivals including Express Scripts, OptumRx and MedImpact, also has a discount card program known as WellCardRx. The WellCardRx program was moderately more difficult to use relative to programs offered by some of its rivals. To access it, the company requires you to enroll and activate it by completing a form requesting some basic personal info including name, address (to identify nearby pharmacies within its retail network) and email address. Visit https://wellcardrx.com/get-a-card/ to enroll. Buried within the mice-type of the WellCardRx website is the info you'll need to enroll and to activate your card. For example, you'll have to write-in (or type-in on the online form or app) a "Referring Group ID". If you don't have a "Referring Group ID" (and most people won't unless their employer insurance plan-sponsor has hired Welldyne as its PBM), the "default" value for this field is: WDRXDEF. The company also says that for the "Member ID" field, individuals should use their 10-digit phone #, followed by a 2-digit person code, and those codes include: 01=Member, 02=Spouse, 03=Dependent, etc. To search prices on WellCardRx website, visit https://wellcardrx.com/start-saving-now/pharmacy-savings/ and go to the paragraph marked "Discount Pricing Tool" and select the link to see discount price estimates for prescription drugs in your area. It notes: "Discounted prices are estimates. Savings will be calculated at time of drug purchase." In other words, verify with your pharmacist what the price with the WellCardRx coupon will actually be. Beware: you will be asked to enter the drug's name (also beware that some drug names cannot be found; if they cannot, try searching under the brand-name or drug class such as "insulin" until a name comes up automatically on the website or app) and you'll also need to enter the drug dosage/strength, frequency of dosage, how many units of the drug you're buying (such as tablets, vials, bottles, etc.), how frequently you refill the script, and your zip code. WellCardRx will then provide a list of about 5 pharmacies in your geographic area (based on zip code) plus its own mail-order pharmacy. The search functionality is not very user-friendly.
CapitalRx Advantage Savings https://capitalrxadvantage.com/ is from a rapidly-growing startup PBM known as Capital Rx competing with the likes of Cigna's Express Scripts, United Healthcare's OptumRx and CVS Health's Caremark PBM business. However, CapitalRx operates a unique NADAC cost-plus pricing model for its clients (and by extension, via its coupon-generating website/app), charging its PBM clients a fixed, flat fee per prescription claim processed rather than "spread pricing" (PBM arbitrage) proprietary rebates off the average wholesale price or wholesale acquisition cost.
ScriptHero https://www.scripthero.com/ A relative newcomer (as of 2017) was the addition of one operated by drug wholesaler McKesson, which has a small, but relatively new discount coupon site/app called ScriptHero (through CoverMyMeds, which McKesson acquired in 2017); this option is powered by internally via CoverMyMeds, as well as SingleCare and the MedImpact PBM-powered website/app known as ScriptSave WellRx. As for patient prices on prescription drugs, ScriptHero is (like many of the others) hit-or-miss. Interestingly, I have found ScriptHero to deliver lowest prices on some unexpected medicines (perhaps due to McKesson's CoverMyMeds), therefore I recommend you included it in your search. But by combining several different inputs (including the SingleCare model, the PBM-driven model empowered by MedImpact, along with McKesson's own CoverMyMeds), it hopes to provide a more comprehensive Rx drug coupon-generating website/app and serve its community pharmacy client base as well. Patients may wish to consider using ScriptHero when it offers them the most attractive pricing. Some generics are priced very well with this option given its combo of PBM + SingleCare models deployed, and it offers discounts on many therapeutic classes of prescriptions.
Another factor to consider is Medicare drug plans.
There, many patients on Medicare subscribe to a supplemental plan sometimes referred to as a "Medigap" policy which they pay premiums for to receive additional benefits, such as avoidance of the proverbial Medicare "Donut Hole". There are stories about patients enrolling in such supplemental Medicare drug plans, and patients experiencing the prices that were promised during Medicare open enrollment can rise within a month (see https://www.npr.org/sections/health-shots/2022/05/03/1095946813/medicare-drug-costs-spike for one such example).
But the solution may be remarkably similar: bypassing your Medigap policy and paying cash for certain drugs without ever submitting a Medicare claim. Patients sometimes find it a hassle and some pharmacy techs don't realize they are not obliged to submit drug purchases to a Medicare drug plan because they're used to everyone on Medicare being handled a specific way.
On generics, in particular, the effort may be well worth simply bypassing your Medigap plan. It is all part of the same dysfunctional "system" (a misnomer if ever there was one). While my example was with a commercial healthcare insurance plan, its easy to envision something similar happening to Medicare patients.
The FTC Is FINALLY Now Investigating PBM Wrongdoing
The FTC's unanimous (5-0) decision to formally study the prescription drug middleman https://www.ftc.gov/news-events/news/press-releases/2022/06/ftc-launches-inquiry-prescription-drug-middlemen-industry) demanding data from the six largest Pharmacy Benefit Managers or "PBM's" and seeking information and records regarding their business practices is likely to eventually yield info about the impact that vertically integrated Pharmacy Benefit Managers has on public access and affordability of prescription drugs. But the study will take some time to actually gather necessary information, although the FTC demands for information are effectively subpoenas which can result in significant fines from FTC if the PBM's fail to comply. Ultimately, however, it will require action from both the FTC and the U.S. Department of Justice to litigate and resolve the underlying wrongdoing.
Meanwhile, the FTC has also formally put the drug companies (like Novo Nordisk) who pay massive "rebates" for exclusive formulary placement, and the PBM's who aggregate such rebates for the insurance companies that own them that it intends to examine possible anti-competitive practices by Pharmacy Benefit Managers (PBM's) with respect to the use of rebate arrangements ("rebates" cash are payments from drug manufacturers to PBM's in exchange for moving market share towards preferred products on the formulary. PBM's and the drug companies regularly pay legally-exempted kickbacks in the form of "rebates" for exclusive formulary placement, but FTC is saying such behavior may actually be in violation of several U.S. laws, including Section 5 of the FTC Act, Section 3 of the Clayton Act, Section 2 of the Robinson-Patman Act, and the Sherman Act to name several (see the new policy statement at https://www.ftc.gov/system/files/ftc_gov/pdf/Policy%20Statement%20of%20the%20Federal%20Trade%20Commission%20on%20Rebates%20and%20Fees%20in%20Exchange%20for%20Excluding%20Lower-Cost%20Drug%20Products.near%20final.pdf for details).
Patients are therefore forced to await the FTC outcome, because it seems very clear wrongdoing is taking place, and at least now the right party is finally investigating. In the meantime, at least one-in-four of us find using the PBM-powered coupon workaround can yield some rather significant savings of 55% to 85% savings; and I encourage readers to consider my own experience as an example.






























No comments:
Post a Comment